Men and cancer: How to recognize three forms and how they are treated
kdriscoll@vaildaily.com
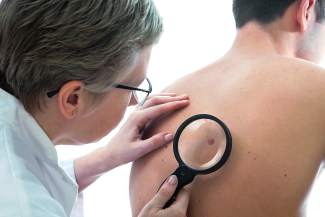
Getty Images/iStockphoto | iStockphoto
Editor’s note: This is the third part of a three-part series on men’s health. Read the first two articles in the series at http://www.vaildaily.com.
Non-melanoma skin cancers are the most commonly diagnosed cancers in men. They’re divided into two main categories: Basal cell carcinoma is the most common, followed by squamous cell carcinoma.
“They originate from different parts of the epidermis, the top layer of skin,” said Dr. Karen Nern, board-certified dermatologist at Vail Dermatology in Edwards, adding that most are attributed to sun exposure, environmental damage or genetics. “Irish, Scottish and English heritages are more likely to get these skin cancers than other skin types.”
Basal cells are typically slow-growing tumors that are often mistaken for pimples that won’t go away or a spot that bleeds easily. To the patient, it can feel like the symptoms come and go, when really the tumor is continuing to grow very slowly, Nern said.
“They can look like a pink spot or a white spot or a scar,” she said. “They can have some color to them, but most of them are pink or white. They can frequently grow undetected for a year or two before people notice them; they can be very subtle. The squamous cancer tends to be tender — they hurt; they’re not very subtle.”

Support Local Journalism
Treating skin cancer
Once diagnosed, basal and squamous cells can be treated with topical medications, scraping or excision, where the cells are cut out and the skin stitched back together. Nern also practices a type of skin cancer removal called Mohs, named for Dr. Frederick Mohs, who developed the surgery in the 1930s.
“I will take it out like taking the bad spot out of an apple, leaving the smallest possible scar,” Nern said. “Then I check it under a microscope to make sure that the edges are clear, and if they aren’t clear, I can take some more wherever it’s positive. I do over 500 of those a year in the mountains. For skin cancers on the head and neck, Mohs is really the treatment of choice.”
Non-melanoma skin cancers are much more common in men than women, particularly men older than 50, and they tend to be more aggressive, leading to a higher mortality rate for men than women. Genetic predisposition can contribute to a higher risk for these cancers, but behavior has a much larger impact, Nern said.
“If you look at genetic populations from England and Australia, they’re the same genetics, but there’s a five-times greater risk in Australia than England because of behaviors,” she said.
To reduce the risk of developing non-melanoma skin cancer, Nern advised limiting sun exposure during peak ultraviolet hours, about 10 a.m. to 2 p.m., and covering up when you do go out, whether it’s with clothing or sunscreen.
“If people are going to be out skiing in intense sun, wear a face mask protector,” she said. “If you’re out fishing, wear a long-sleeved shirt. There are a lot of companies that make UV clothing that’s lightweight. There’s even a laundry detergent additive you can add to clothing to make it have better UV protection.”
Choose a sunscreen that provides both UVA and UVB protection, preferably one that contains zinc oxide, she said, which sits on top of the skin, rather than being absorbed, creating a barrier that reflects and scatters UV rays.
“Use them every single day, no matter whether you’re going to be out or not,” Nern said of sunscreens. “You get exposure through car windows and other places, and accumulative exposure increases skin cancer risk.”
About one in five people will get skin cancer in their lifetime, and men have a higher risk of developing it than women, Nern said.
“They spend a lot of time outdoors and are less likely to use sunscreen to protect their skin,” she said. “Women cover their skin with makeup, which has a little bit of protection, even if they’re not using sunscreen.”
Prostate, testicular cancers
The second most commonly diagnosed cancer for men is prostate cancer, though it’s more difficult to detect than other forms of the disease because the prostate is not amenable to self-exam, said Dr. Alec Urquhart, medical director of medical oncology at the Shaw Regional Cancer Center.
“It is not easily palpable and is best done by digital rectal exam by a physician,” he said. “But even this only assesses cancers in the posterior portion of the prostate. PSA (prostate-specific antigen) is a blood test can be done to screen, as well, but this is not always perfect. There are some men with elevated PSA who do not have prostate cancer and other men who have prostate cancer with normal PSAs.”
Sometimes men can present with symptoms, but that can be late in the development of the cancer, he said. Ultimately, the diagnosis is made by a specialized biopsy of the prostate, and treatment depends upon how large the cancer is, if it has spread to adjacent structures or beyond and how aggressive it appears on the biopsy.
“It can be treated with surgery or radiation alone,” Urquhart said. “More advanced disease can be treated with combinations of surgery, radiation and anti-hormone therapies that block testosterone. In older men with very low grade cancers, sometimes it can be watched closely.”
While it is true that many prostate cancers are slow growing, others can be very aggressive, so early detection is important, as is discussing screening with your physician.
Navigating the research about what men can do to prevent prostate cancer is difficult, Urquhart said, but evidence suggests that diet may influence risk.
“Recommendations include low-fat diet, with a preference for plant-based fats, lots of fruit and vegetables and including fish in your diet,” he said. “It is also noted that obesity is associated with a higher risk for prostate cancer, so it’s important to maintain a healthy body weight. Regular exercise has been associated with a lower risk of prostate cancer, too.”
Unlike prostate cancer, there is no data for preventing testicular cancer, Urquhart said. Some doctors suggest regular self-exams as a way to catch it sooner. If a mass is discovered, screening for cancerous tissue includes an ultrasound of the mass, as well as blood tests and scans.
“Treatment is typically first surgical, with removal of the affected testicle,” the oncologist said. “Depending upon stage of the disease or if there is evidence of spread to internal lymph nodes — detected on CT scan — or other organs, we may treat with chemotherapy. Testicular cancer is typically very sensitive to chemotherapy and even very advanced disease can be cured.”









