Stroke of genius in Vail
Vail CO, Colorado
ALL |
VAIL, Colorado ” Patricia Tisdale woke up in her Eagle-Vail home feeling strange. Her head throbbed. She was dizzy and confused.
“We need to get to the hospital right away,” she told her husband, Doug.
An ambulance whisked Patricia to the Vail Valley Medical Center in Vail, where doctors suspected she was having a stroke.
Doug was stunned. His wife was just 52 with no family history of stroke, no high blood pressure, no weight problems, no smoking habit.
For Patricia to have a stroke seemed surreal.

Support Local Journalism
Medical personnel tried to drive Patricia to see a stroke specialist at a Denver hospital, but traffic and 20 inches of snow forced the ambulance to turn back. A helicopter flew Patricia to the hospital instead, where she remained in a coma.
On Tuesday, Jan. 6, 2004, Patricia passed away as a result of her stroke.
“It was just the most difficult thing I’ve ever had to deal with in my life,” Doug said. “We had been married for 31 years and one week, and it was just something I never, ever assumed that I would have to go on without my wife.”
Doug’s grief hardened into action. A member of the Vail Valley Medical Center’s board of directors, Doug heard about a stroke monitor camera that could put doctors in Vail in almost instant contact with stroke specialists in Denver. He and former hospital CEO Greg Repetti put up the funding for the camera, and in 2006, Vail became the first town in Colorado with the device.
Doug lost his wife, but perhaps the camera could help other men and women who suffer strokes.
“I don’t ever want a guy to go through what I did that Sunday and be as clueless as I was that Sunday,” Doug said.
Most hospitals in Colorado’s remote or rural communities do not admit enough stroke cases to warrant hiring a stroke specialist, said Luanne Williams, executive director of the Colorado Neurological Institute in Englewood. A neurologist makes roughly $150,000 to $200,000 per year, she said. And to provide 24-hour coverage, a hospital would need to hire three of those specialists, she said.
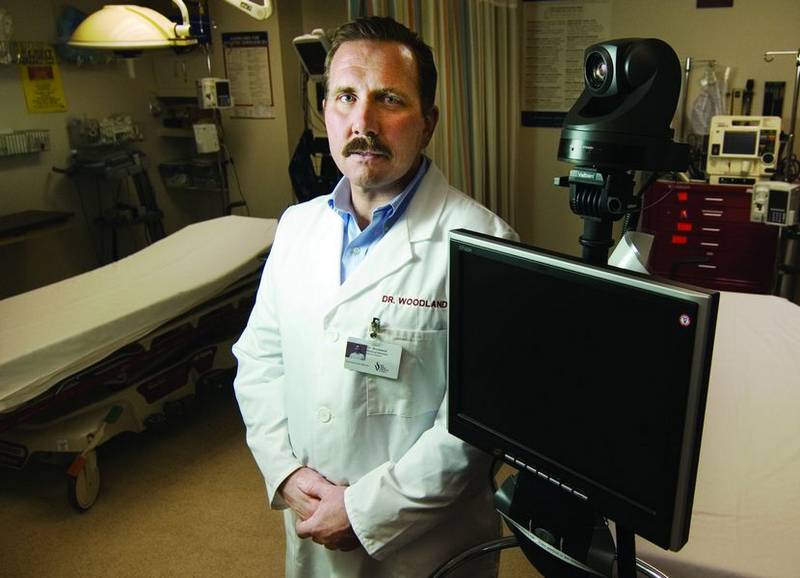
Yet the volume of stroke patients in a small town like Vail is low. Dr. Chip Woodland, an emergency department physician, said roughly one or two patients per month receive a stroke consultation at the Vail Valley Medical Center. The hospital has emergency doctors, who receive training for initial diagnosis and treatment of strokes, and internal medicine doctors, who can admit patients for strokes, but does not employ any neurologists who specialize in strokes.
“Let’s say in Vail, in the course of a year, there are 20 strokes,” Williams said. “It doesn’t make any sense to have three neurologists on the payroll, waiting around for those strokes to happen.”
The Colorado Neurological Institute offers a cheaper solution: A camera that allows doctors in remote towns to consult with stroke specialists at the institute’s Swedish Medical Center in Denver 24 hours per day. The system costs $35,000.
Called CO-doc, the system includes a computer and monitor on a rolling stand. A camera allows doctors in Vail and Denver to consult with one another through real-time video and audio.
In addition, the specialist in Denver can interview the patient in Vail through the camera. The specialist can ask the patient questions, and even move the camera on the patient’s end to examine the patient. For instance, the specialist can zoom in on the patient’s pupil to see whether it’s dilated or ask the patient to raise his or her arms.
With this information the specialist can assist with the diagnosis, suggest treatment ” and help the Vail doctor make a pivotal call.
One of the most important decisions facing doctors treating a stroke patient is whether to give the patient a clot-busting drug.
“It can dissolve the clot, but in a small percentage of patients, it actually makes the stroke much worse,” Woodland said.
With a stroke, blood flow to the brain is interrupted. There are two types of strokes: those caused by a blood clot in an artery and those caused by a tear in the artery.
If an artery bursts or tears, a CAT scan shows blood leaking into the brain, and doctors automatically disqualify the patient for taking the clot-busting drug. That’s because the drug, called a tissue plasminogen activator, or tPA, thins the blood, and would cause the blood to leak faster into the brain.
If the scan shows no blood seeping into the brain, the diagnosis gets tricky. The patient might suffer from a stroke caused by a blood clot. Or, the patient might have one of the many conditions that “masquerade” as strokes, such as Todd’s paralysis, hypoglycemic episodes or the aftermath of a seizure, Woodland said. Tests such as MRI can pinpoint blood clots, but they take too long to be practical, said Chris Fanale, a stroke neurologist with the Colorado Neurological Institute.
That means doctors in Vail lack definite proof about whether a patient is having a stroke. The fear: Exposing the patient to the dangers associated with the clot-busting drug when the patient isn’t even having a stroke, Woodland said. In some patients, the drug can cause bleeding at an ulcer or fragile blood vessel, which can at worst lead to surgery or death, Fanale said. Further clouding matters, not all blood clot patients are candidates for the drug, Fanale said. For example, patients with high blood pressure or those who are on blood-thinning medications fail to qualify.
And the clock is ticking as doctors sort through these details. For the clot-busting drug to work, patients must take it within three hours of the onset of a stroke.
That’s why emergency doctors like to get a second opinion about whether to administer the drug, Woodland said.
“It helps us be able to give it sooner, and feel more comfortable with giving it,” he said.
In the past, emergency room doctors had to make the call on their own or ship patients to Denver for a second opinion ” a trip that could use up the three-hour time window for administering the drug, Woodland said.
Yet with the new camera system, doctors in Vail can get a quick second opinion on giving the drug.
“No one’s saying the physicians there are not able or capable,” Fanale said. “These decisions are sometimes very, very difficult and it’s always nice to have someone that you can call to do certain things. For example, I feel like I would know if someone is having a heart attack but I wouldn’t feel comfortable treating them without a cardiologist.”
About a year ago, Margaret Martin, 82, was walking out of her vacation home in Eagle-Vail when her mouth began to droop on the left side.
At the Vail Valley Medical Center, Martin spoke with Fanale using the stroke monitor camera. The doctor told Martin she was a candidate for the clot-busting drug and outlined the risks.
“I said, ‘Let’s go for it,'” Martin recalled.
Doctors administered the drug and helicoptered Martin to Denver for follow-up treatment. Today, she is fully recovered, back to doing church work and planting flowers at her permanent Texas home. In Martin’s eyes, the stroke monitor camera was a blessing.
“It was wonderful because I wouldn’t have known actually what they were considering doing without his explanations,” she said.
High Life Writer Sarah Mausolf can be reached at 970-748-2938 or smausolf@vaildaily.com.










