Colorado Democrats pass stopgap funding for health insurance subsidies
Lawmakers were able to cobble together $140 million to extend state-level benefits for another year, but are still seeking a long-term solution

Robert Tann Follow
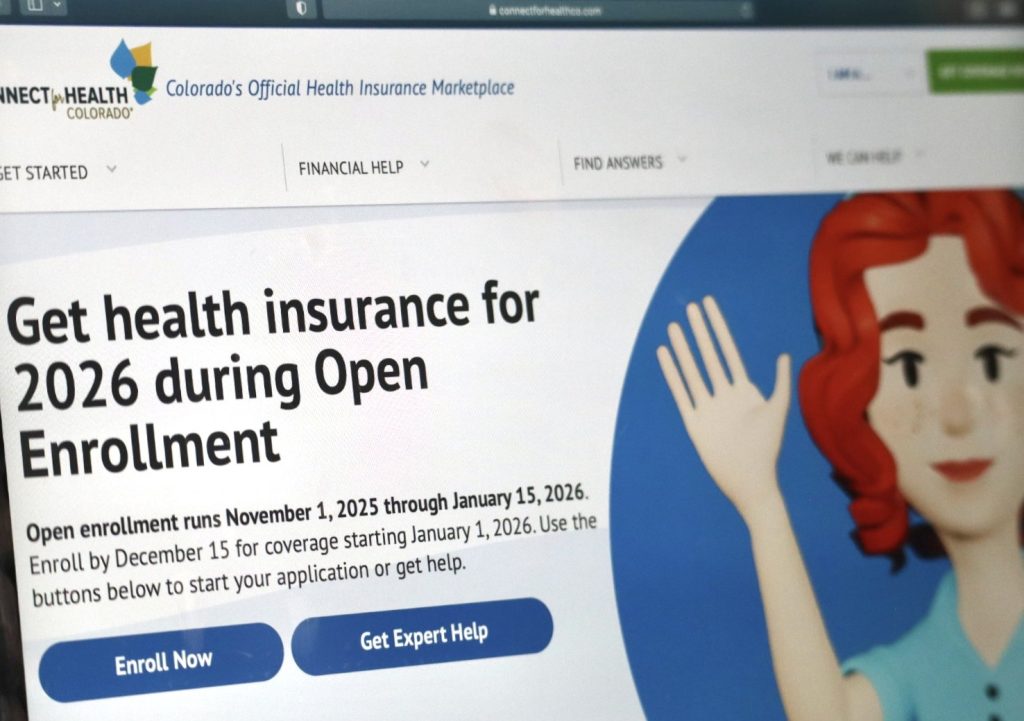
Robert Tann/Vail Daily
Colorado Democrats have approved a stopgap plan to keep health insurance subsidies afloat, but not without prompting concerns from members of both parties about the sustainability of the funding.
Senate Bill 178, which was introduced in the final weeks of the legislative session ending on May 13, would pump $140 million into state health insurance assistance programs following the loss of federal funding. Those programs lower healthcare premiums for people who buy their insurance through Connect for Health Colorado, the Affordable Care Act marketplace, and provide access to commercial insurance plans for immigrants, regardless of their immigration status.
It passed the House on a near party-line vote on Tuesday, May 12, after clearing the Senate along party lines the week before.
The measure underwent several rewrites during the session’s final days as bill sponsors scrambled to find dollars at a time when lawmakers had to slash spending to close a $1 billion budget gap. Even lawmakers who voted for the bill warned that its funding was on shaky ground.
“The funding mechanism for it is just so completely bananas,” said Sen. Jeff Bridges, a Greenwood Village Democrat and member of the legislature’s Joint Budget Committee, during a preliminary vote on the bill on May 8.

Support Local Journalism
Originally, the bill would have siphoned $100 million from the state’s unclaimed property trust fund. That was changed in the final version to allow the state to sell up to $100 million in state bonds, which would be paid back within 45 years. Bonds are sometimes used by governments as a debt-financing tool to generate upfront cash.
The bill would also redirect $40 million in marijuana cash fund reserves to the subsidy programs. Originally, the bill would have raised that money by imposing a fee on major health insurance companies, but that provision was removed after carriers warned it would mean increasing insurance costs on enrollees.
Bridges said he understood the need to help people afford their healthcare, but that he is “deeply uncomfortable with the financing mechanisms.” He called on lawmakers to begin winding down the subsidies, saying the state can’t afford those programs without federal support.
Sen. Barbara Kirkmeyer, a Brighton Republican who also sits on the Joint Budget Committee, said she was glad to see the fee on insurance companies stripped from the bill. But she said there needs to be spending reforms so that “these programs start paying for themselves.”
The measure is the latest attempt by Democrats to blunt the rise in insurance costs caused by the expiration of federal tax credits last year, which helped lower premiums for Affordable Care Act plans. Without those subsidies, some marketplace enrollees reported increases in their monthly premiums, with mountain town residents seeing costs surge by as much as 400%.
During a special session last August, lawmakers approved $110 million in one-time funding for the state’s health insurance assistance programs, which is set to last through 2026. This year’s bill would extend funding through the end of 2027.
Sen. Kyle Mullica, a Thornton Democrat and one of the bill’s lead sponsors, said he and other lawmakers had worked for months to find a more sustainable funding solution. That included an idea to increase the fee insurers already pay to support state subsidies, which was rejected by insurers.
Mullica acknowledged that his bill amounts to a one-time fix, but said it is necessary to mitigate higher insurance premiums that could lead people to forgo coverage.
“Ideally, we would like to see long-term solutions, and, unfortunately, we haven’t been able to get there,” Mullica said during the bill’s final Senate vote on May 9. “… That doesn’t mean that we’re not fighting to make sure that real people in our communities continue to have access to healthcare.”
Bill sponsors agreed to an amendment pushed by Kirkmeyer that would require the State Department of Regulatory Affairs to impose a premium on healthcare plans in 2027 for immigrants enrolled in the state’s OmniSalud program. Currently, OmniSalud offers plans with $0 premiums for low-income immigrants, which Kirkmeyer argued was unfair and a source of the program’s funding issues.
The bill was also amended to reduce the financial burden of the state’s reinsurance program, which helps lower premiums. Currently, the program is required to reduce statewide average premiums by 20%. The bill changes that requirement to 18%.